Coronavirus - Screening for Elevated Body Temperature - MoviTHERM
The Coronavirus outbreak in Wuhan, China has grabbed the attention of people around the globe. Thermal cameras are being deployed in record time for screening of elevated body temperature at airports and other public places.
However, as useful and capable as this technology is, there is a lot of misinformation circulating in the news. As with the implementation of any technology, there are challenges. It is important to understand the physics involved that affect the accuracy of an optical temperature measurement, but moreover, there are many other factors to consider related to bio-physical phenomena.
Being unaware of how these intricate details is crucially important.
Knowing what works and why it works can make the difference between having a cool looking piece of equipment and an effective tool that assists in the screening effort. – adds Markus Tarin, President & CEO, MoviTHERM
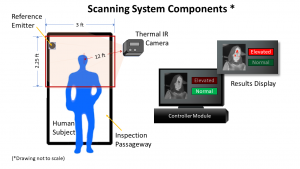
 We commonly see thermal imaging system setups that simply point a thermal camera into a crowd. This sort of setup is significantly flawed, when considering all factors that contribute to the accuracy of measuring human elevated body temperature.
We commonly see thermal imaging system setups that simply point a thermal camera into a crowd. This sort of setup is significantly flawed, when considering all factors that contribute to the accuracy of measuring human elevated body temperature.
More specifically, how skin facial temperature correlates to core body temperature. Based on scientific research (referenced below), the most reliable spot in the human face is the eye canthus.
A small area over the tear duct. The eye canthus is strongly correlated to the inner body core temperature and has been found to the most reliable location on the face.
Image: Courtesy of Ross Overstreet, Flir Systems, Inc.
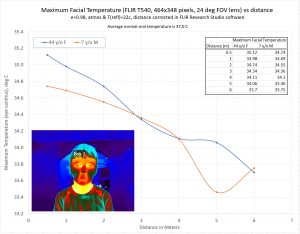
The image to the left shows the relationship between the camera distance to subject and the measured skin temperature. Two subject were used, a seven year old male and a 44 year old female. Both subjects were imaged under the same conditions.
Moving the camera from 0.5 meter to 6.0 meter away from the subject, resulted in a temperature drop of about 2 degrees Celsius. This is due to the decreasing resolution of the number of pixels projected over the eye canthus, when moving the camera further away from the subject. Compounding this issue is the fact that the standard accuracy of a thermal is only +/- 2 degrees Celsius to begin with. These sort of issues, when compounding would lead to a greater than 50% uncertainty in the screening system at best.
Sufficient number of pixels (spatial resolution) is required for a thermal camera to accurately measure the skin surface temperature. With the limited amount of pixel resolution available, this poses a challenge when imaging a subject, even at a modest distance. Most cameras deployed for elevated body temperature screening have a resolution around 320 x 240 pixels or 640 x 512. This is very low when compared to traditional surveillance cameras. The FLIR A320 Tempscreen camera was specifically designed for this application.
Rather than using a reference temperature source (“black body”), the FLIR A320 Tempscreen uses a different approach to assuring the skin surface temperature measurements are as accurate as possible. For this, the FLIR A320 Tempscreen uses a population baseline. FLIR suggests using about ten known healthy individuals, scan them with the camera and save their readings. All future subjects scanned will be compared to this population baseline.
A better (and necessary) approach to solving the resolution vs. distance challenge is to control the distance to the subject. This is not feasible when pointing a camera into a crowd. The following setup would create a more controlled measurement setup. Since the accuracy of most thermal cameras are only +/- 2 degrees Celsius to begin with, another step has to be taken.
A calibrated temperature reference needs to be placed in the field of view during the measurement. The reference source, also referred to as a “black body” allows the imaging software to calibrate the scene to a more precise value by providing a higher accuracy reference, than the camera is capable of.
The black body needs to be located at the same distance from the camera, as the face that is being imaged. The active area (heated region) of the black body also needs to be covered with sufficient pixels to yield the desired results. Ideally a pixel cluster of 10 x 10 pixels.
With this approach, temperature measurements of 5 to 10 times the NETD of the camera are possible. Or about +/- 0.5 degrees C. Cameras that support a black body as a reference source are the new FLIR A400 and FLIR A700 Smart Sensor cameras.
This video explains how thermal imaging technology can be used to screen for people with an elevated body temperature. We have seen a lot of misinformation lately from sources claiming that you can simply point a thermal camera into a crowd and “detect” anybody infected with the Coronavirus.
We want to set the record straight and explain the technology in layman’s terms. How thermal cameras work; how you can use thermal imaging to measure skin temperatures and what you can and cannot detect.
There are also several pitfalls and challenges with this technology when it comes to detecting somebody with an elevated body temperature. Things that can affect the accuracy of the measurement are:
- Makeup
- Physiological Stress
- Sweating
- Insufficient Camera Resolution
- Measuring the wrong location on the face
- Not using a reference black body for calibration
- Using the wrong camera
- Subject motion
… just to name a few.
Related Scientific Research
Below are some research papers that take a deeper dive into the challenges that are being discussed in this video.
Best practices for standardized performance testing of infrared thermographs intended for fever screening. Pejman Ghassemi,T. Joshua Pfefer, Jon P. Casamento, Rob Simpson, Quanzeng Wang. September 19, 2018 https://doi.org/10.1371/journal.pone….
International travels and fever screening during epidemics: a literature review on the effectiveness and potential use of non-contact infrared thermometers. Bitar D, Goubar A, Desenclos J C. Euro Surveill. 2009. https://www.ncbi.nlm.nih.gov/pubmed/19215720
Comparison of Infrared Thermal Detection Systems for mass fever screening in a tropical healthcare setting, M.R. Tay, Y.L. Low, X. Zhao, A.R. Cook, V.J. Lee ,Public Health, 2015. https://www.sciencedirect.com/science/article/abs/pii/S0033350615002838.
Infrared thermal imaging of the inner canthus of the eye as an estimator of body core temperature. Teunissen, L. P. J., & Daanen, H. A. M. (2011). Journal of Medical Engineering & Technology.. https://doi.org/10.3109/03091902.2011…